The Uetrecht Family
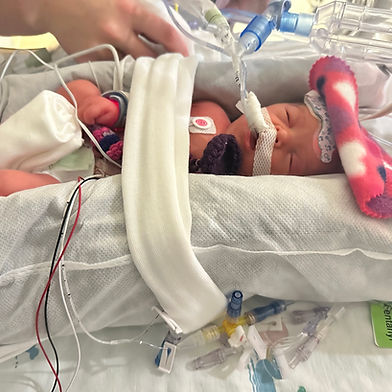
Baby Valerie
Relocated from Jonesburg, MO to Kansas City, MO (200 miles)
Scroll down to see updates as the Uetrecht family progresses in their CDH Journey! (All updates are written and given by parents with consent)
Initial Backstory
"On September 12th, 2025, the day before our 9th wedding anniversary, my husband and I went to the anatomy scan for our fourth child. We were so excited to see our baby for the first time, and maybe find out the gender. We were undecided. The tech came in and started our scan. We casually chatted about our faith, children, and lives. It felt like the scan was taking forever then she stepped out, saying she’d return in a couple minutes. Twenty minutes later she came back in and told us the scan was complete but we needed to meet a doctor in the next room over. This was very odd because we were under care of a midwife not associated with this office. I looked at my husband and told him “something isn’t right. I’ve had three anatomy scans here and never met a doctor.” He was hopeful and reassuring that everything was fine. We made it to the next room and met with an offsite doctor via iPad-STRANGE! She came on and told us that everything looked good with baby except the placement of her stomach, it was too close to her heart. We were then referred to a major STL children’s hospital. The following week we went and met with the doctor in STL. After an ultrasound the tech recorded her heartbeat and put it in a bear; this couldn’t be good- right? The doctor came in and told us that she had a severe left side CDH. A large hole with minimal diaphram. Her stomach and bowels were in her chest and her liver was creeping up. He told us that if her liver creeped in more she wouldn’t live. He said with her current LHR she had an estimated 5% survival chance. He proceeded to tell us that if he did not work at a catholic hospital he would recommend terminating our pregnancy. He also told us we could go to Boston or St.Petersburg for fetal surgery that would help but not guarantee life. We left there absolutely devastated! We left really thinking we’d never hold our baby alive. With three young kids at home there was no way I could relocate to Florida or Massachusetts. That afternoon I found Dr. Lobeck and Dr. Vricella at Children’s Mercy in Kansas City, MO. Dr. Lobeck was performing the FETO procedure in the Midwest, just a few hours from home! The following Monday we traveled to Kansas City and met with a huge team. Long story short, our baby qualified for FETO and Dr.Lobeck would do it. I relocated away from my husband and children on October 24th, had fetal surgery on October 27th. I left the hospital a couple days later and went to a local hotel. Settled in to stay-hopeful not to return to the hospital until balloon pop mid-December! Valerie had a different plan. My water broke on November 3rd and I was admitted to the hospital. They closely monitored us until November 11th when they decided that an emergent EXIT procedure was necessary. She was only 29w5d gestation. Everyone told us she’d need to be 34w for ECMO and they predicted a need for it. We were so scared. Valerie was triumphant. She was born 3lb6oz, put on the oscillator, and settled into her spot in the ECMO suite even tho she wasn’t big enough for it. Turns out she wouldn’t need ECMO. She was stable and remained pretty stable. SIX weeks and four days later she was finally ready for her repair surgery! She did wonderful, her surgeon sewed in a beautiful patch. Three days later she failed extubation and scared mom and dad big time! They reintubated and she stabilized. On January 8, 2025 she decided she was done with the vent and caused a dramatic stir in the NICU. She self extubated and she BREATHED! She’s on low cpap settings for now and doing fantastic. We are so grateful for our miracle baby."
Update 2/2/2026
Valerie stayed extubated and thrived on CPAP. They slowly weaned her settings until she transferred to high flow oxygen. 5liters and 21% to start out. She’s made her way to 2liters of high flow oxygen which means it’s time to start oral feeding! We started breastfeeding on 2/1/26 and she’s done fantastic so far. We gotta keep gaining weight while breastfeeding, transfer to room air, and maintain stats then we’re real close to walking out of this hospital!
Update 3/1/2026
Valerie made her way onto room air and did wonderful! She appeared to be doing great eating but was struggling to gain weight so a swallow study was advised. She was unorganized and aspirating so we started thickened feeds. She tolerated the switch well and gained weight so she we got discharged on 2/28/26! We are so happy to be out of the NICU!